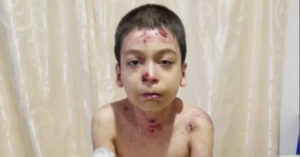
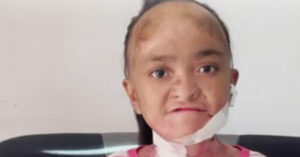
In a brand new study that was published in the Journal of Central Nervous System Disease, a few researchers from North Carolina State University talk about an adolescent diagnosed with rapid onset schizophrenia who was later found to have Bartonella henselae infection.
Bartonella is a bacteria that is frequently known for its role in cat scratch disease.
The new discovery adds to the growing mountain of evidence that Bartonella infection can create a number of chronic health conditions, including mental illness, and could open up new roads for research into bacterial or microbial root-causes of psychiatric issues.
There are at least 30 varieties known species of Bartonella, and 13 of these have been found to affect humans. Until recently, the bacteria was believed to be a short-lived (or self-limiting) infection.
Bartonella is infamous for “hiding” in the linings of blood vessels, but with the creation of new, more specific diagnostic tools, the bacteria has been discovered in the blood or cerebrospinal fluid of patients with a variety of neurological symptoms. In fact, Bartonella has been spotted in individuals diagnosed with chronic illnesses such as migraines to seizures to rheumatoid illnesses.
In this example, an adolescent who had sudden-onset psychotic behavior was initially diagnosed with schizophrenia. The patient was seen and treated by numerous specialists and therapists over an 18-month timeframe; however, all typical conventional treatments for both psychosis and autoimmune disorders were ineffective.
Finally a physician noted that the patient’s skin lesions were those often associated with the Bartonella infection. The patient tested positive for the bacteria and was prescribed combination antimicrobial chemotherapy which led to a full recovery.
“This case is interesting for a number of reasons,” said Dr. Ed Breitschwerdt, Melanie S. Steele Distinguished Professor of Internal Medicine at NC State and lead author of the case report.
“Beyond suggesting that Bartonella infection itself could contribute to progressive neuropsychiatric disorders like schizophrenia, it raises the question of how often infection may be involved with psychiatric disorders generally,” he said.
“Researchers are starting to look at things like infection’s role in Alzheimer’s disease, for example. Beyond this one case, there’s a lot of movement in trying to understand the potential role of viral and bacterial infections in these medically complex diseases. This case gives us proof that there can be a connection, and offers an opportunity for future investigations.”
Source: North Carolina State University